Should you Jefferson Curl?
I recently was listening to a Tim Ferris podcast, and he had on Coach Sommer. Coach is founder of GymnasticBodies and a former US National Gymnastics Coach. Fair to say that he has a ton of experience and a wealth of knowledge. When asked if he had to prescribe 3-5 exercises/stretches for common deficiencies typically seen, Coach Sommer named the Jefferson Curl (JC) as numero uno. Earlier in the podcast he justified his use of this controversial exercise by saying, (1) Stu McGill’s research was done with dead tissue, so obviously it doesn’t adapt to increasing stress and (2) he has been using this move for 10-15 years without issue.
This definitely made me put down my sardines. Coach Sommer prescribing such a risky move for the general population definitely peaked my attention. Here is a world class coach telling the majority of people they should be performing this move. His reasoning based completely on experience and a dismissal of a single data point. We will talk about evidenced based practice in a bit, but definitely clinical experience is one of the pillars, and a very important part.
BUT… and a big but…
With all due respect, Coach Sommer is definitely making a mistake by justifying the JC by dismissing Dr. McGill’s work. Of course dead tissue doesn’t respond and adapt, but this is just one piece of a pretty strong data driven argument against loaded flexion.
All that said, lets get a better understanding of the JC.
So what is The Jefferson Curl?
The JC is multi-segmental flexion under load. Typically with weight in hand and standing on elevated surface to pass restriction of floor. The idea behind the move is to increase your resiliency to loaded flexion. The exercise is started with extremely light weight and progressed over a year or two to near bodyweight.
Evidenced Based Reasoning
As I said earlier, we need criteria to justify using a particular component in our training. We can use the father of evidenced based practice, Dr. David Sacket’s criteria. He described 3 tenets or pillars to evidenced based practice…
- Best Research Available
- Clinical Expertise
- Patient Values
It is important to note that all of these stand together and no one tenet is more important than the other. Over the next couple of blogs we will use this as our measuring stick when deciding whether or not to implement the JC into our training program.
Lumbar Spine Anatomy
In order to have an “intelligent” conversation, we have to understand the anatomy we are talking about. Here’s a quick review of lumbar spine anatomy.
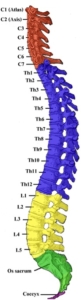
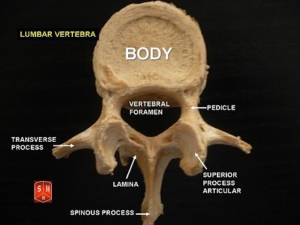
The Lumbar Spine consists of 5 segments L1-L5. Anatomically the lumbar spine has thicker/wider bodies than the rest of the spine. That is a common theme with the Lumbar Spine in that it is thicker and wider. This is important because it has to be a load bearing structure. Pay attention to the pedicles and the spinous process. Again these are very hardy and allow for compressive forces to be displaced and absorbed.
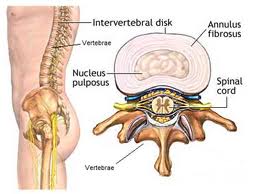
Between each vertebrae sits a disc. The central portion or Nucleus Pulposis is like a pasty water and surrounded by a much thicker outer layer of collagen, referred to as the annulus fibrosis. This annulus and nucleus both contain type II collagen, but the outer annulus contains more type I collagen in concentration. Why does this matter? Type I is more often seen in tendons, skin, and artery walls. So type I has more of an elastic component to it. Type II collagen is typically found in cartilage and is less stretchy and more rough.
The 3 motions allowed for at the lumbar spine are flexion/extension, rotation, and side bend. The majority of motion allowed at the lumbar spine is flexion and extension. Very little rotation or side bend is allowed for at the lumbar spine without running into the mechanical restrictions.
Conclusion
In future discussions we will discuss positions for and against the JC. Checkout part 2 where we will make an evidenced based argument against the JC using Dr. Sacket’s pillars of evidenced based practice.

For Brandon, fitness has been his passion for as long as he can remember. In high school he was a three-sport athlete and received a scholar athlete award in football. Later, he attended Arizona State University on an academic scholarship and received his degree in Kinesiology in 2004. When he was a junior in college, he started Personal Training and has since turned this into his career. Brandon is a natural teacher who is passionate about health, fitness, wellness, and life. Each and every day he feels blessed to be able to do what he loves most…help people achieve a healthier life! Working with his best friend and having clients who he considers to be his family is one of the best jobs he could ever wish for. What he loves most about being a personal trainer is helping his clients achieve what they thought was the “impossible”!
Brandon’s philosophy is that exercise and fitness should be viewed as preventive medicine. If one takes care of his/her body today, he/she will stay healthy for the remainder of his/her life. His main focus is on functional training that incorporates normal daily movements which strengthen core muscle groups and help deliver a functionally fit body. This body will then be efficient with all activities, from athletics to everyday movements.



But why is it called a Jefferson curl?